Your Family Deserves the Best Care Book an Appointment
Your skin health matters, so don’t delay. Our clinicians look forward to treating you and your family at one of our local New England practices.
Find Your Nearest APDerm Center


Verrucae plantaris, also known as plantar warts, are warts that typically develop on the soles of the feet. Plantar warts manifest as small, grainy growths with a rough texture and they can also display minuscule black dots at their core, representing clotted blood vessels. While plantar warts are typically not harmful, they can cause discomfort and are more prevalent in children, adolescents, and individuals with compromised immune systems. It is crucial to understand that although plantar warts and seed warts, as well as common warts and seed warts, have distinct differences, they also share many similarities.
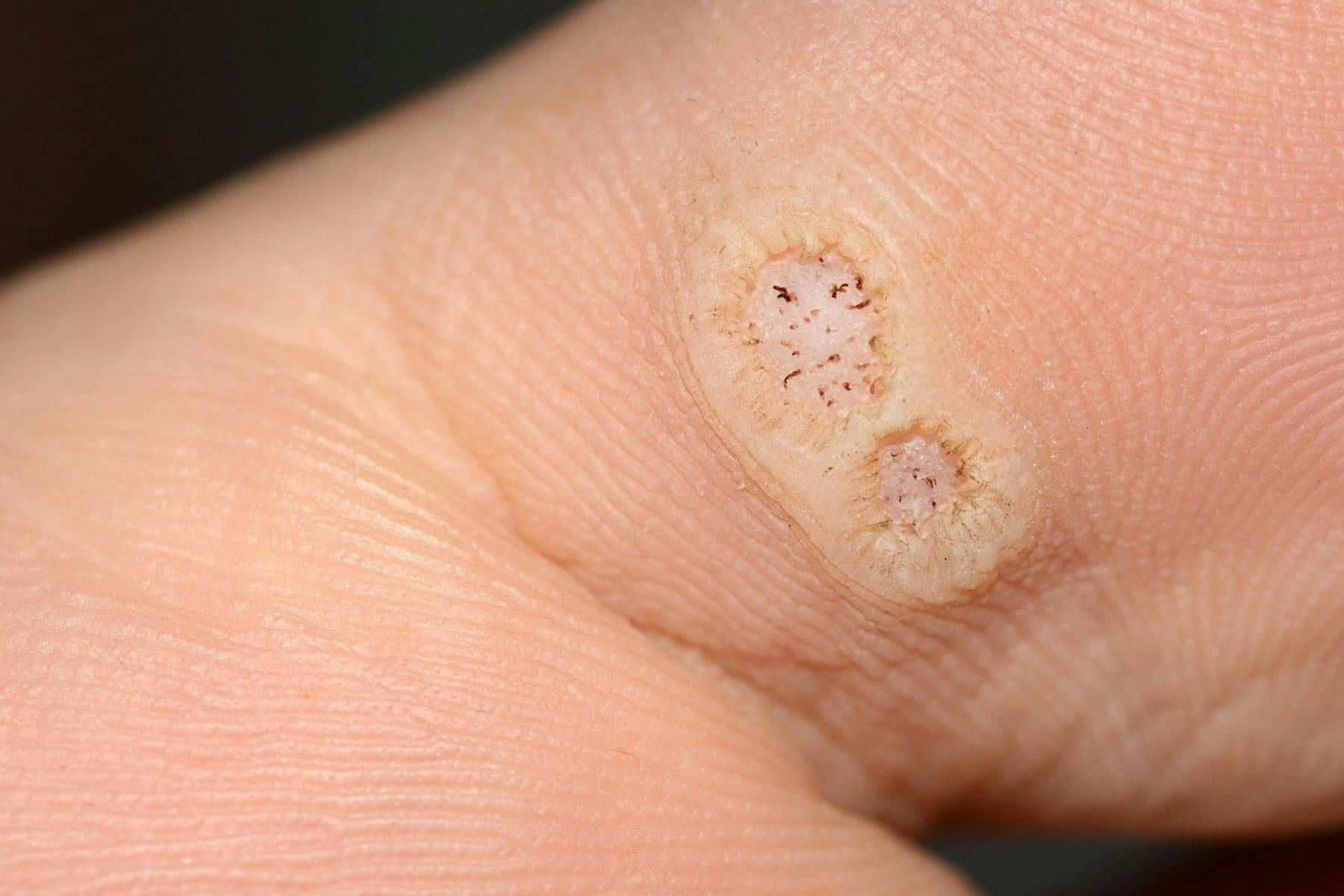
These distinguishing factors can include the location and appearance of the wart, the level of discomfort, and the wart treatment options. Therefore, seeking a professional opinion to accurately diagnose your warts is of the utmost importance. For example, the appearance of tiny black dots resembling seeds can be found in common warts, seed warts, and plantar warts. However, what distinguishes the type of wart is the specific human papillomavirus (HPV) strain responsible for causing it, as well as the most appropriate treatment approach.
The HPV strain that causes plantar warts thrives in warm and moist environments, similar to seed warts, and both plantar warts and seed warts can be treated using similar methods – these include topical treatments, cryotherapy, or surgical removal performed by a healthcare professional.
Therefore, to prevent potential complications, it is vital to book an evaluation with a healthcare professional for accurate diagnosis and appropriate treatment.
Plantar warts exhibit various noticeable characteristics, and the severity thereof can differ from person to person – thus, it is crucial to understand that not all plantar warts will display the same level of symptoms, and some may be more troublesome than others.
One of the primary plantar wart symptoms is the thickening of the skin over the affected area. Due to constant pressure and friction from walking and standing, the skin in the region of the wart can become hardened and calloused. This thickened skin serves as a protective response by the body to reduce pain and discomfort. The skin essentially acts as a cushion, shielding the underlying tissues from direct pressure and minimizing the irritation caused by the wart’s presence.
Typically, plantar warts manifest as small, grainy lesions located on the sole of the foot. They can have a rough surface texture and in some cases, they can feature well-defined borders that set them apart from the surrounding skin. Plantar warts may display various colors, ranging from flesh-toned to gray or brown, and the color is mainly determined by the presence of blood vessels within the wart and the thickness of the overlying skin. It does not necessarily indicate the wart’s type or severity.
A characteristic feature of plantar warts is the presence of tiny black dots within the lesion, often referred to as “wart seeds.” These black dots are clotted blood vessels that have become visible due to the wart’s growth and the pressure exerted on the foot. However, this characteristic can cause plantar warts to become confused with seed warts, which is why seeking a professional diagnosis is so important, especially when deciding on the most effective method of plantar wart treatment.
While not all plantar warts cause substantial discomfort, some individuals may experience pain or tenderness in the affected area, especially when walking or standing and with increased pressure on the wart. This is because plantar warts can grow inward, beneath the skin’s surface, which can irritate nerve endings and contribute to the pain experienced. As the plantar wart progresses, it can lead to the stretching and distortion of the surrounding skin tissues, resulting in tenderness.
Plantar warts can vary in size, and they occur as solitary growths or in clusters known as mosaic warts. Mosaic warts are groups of closely spaced plantar warts that merge, forming a larger, irregularly shaped patch on the foot. This can occur due to continuous foot pressure and is also more prevalent in individuals with weakened immune systems or those who frequently walk barefoot in public areas, facilitating easy virus transmission.
If you have concerns about plantar warts or questions about plantar wart treatments, it is crucial to seek medical advice from a healthcare professional. Without a proper plantar wart diagnosis, it can be difficult to pinpoint an appropriate treatment plan for plantar warts and increase the risk of potential complications. Healthcare providers can suggest suitable plantar wart treatment options tailored to the severity of your condition and medical history.


The human papillomavirus (HPV) causes plantar warts, medically known as verrucae plantaris. HPV is a highly contagious virus that can infect the outer layer of the skin and lead to the formation of warts. Among the numerous types of HPV, only a few strains are responsible for causing plantar warts – these include HPV types 1, 2, 4, 60, and 63. Plantar warts are caused by an HPV infection in the outer skin layer on the soles of the feet. The virus thrives in warm and moist environments and commonly enters through small cuts, breaks, or abrasions on the bottom of the foot when walking barefoot in public areas like showers, swimming pools, and communal spaces. Once the HPV infects the skin cells on the soles of the feet, it triggers abnormal growth, leading to the formation of a plantar wart. The virus essentially enters the outer skin layer, known as the epidermis, and integrates into the genetic material of the skin cells – this disrupts their normal division and replication processes, causing rapid cell multiplication and the accumulation of infected cells.
Due to the inward growth pattern caused by the virus, the wart becomes less recognizable to the immune system, making it challenging for the body to eliminate the infected tissue effectively. Consequently, untreated plantar warts can persist for extended periods. What makes the virus particularly contagious is that it can be transmitted through direct contact with infected surfaces or by coming into contact with the skin of someone who has plantar warts. Seeking appropriate medical attention is crucial to address plantar warts effectively and prevent potential complications.
Diagnosing plantar warts requires a thorough evaluation by a healthcare professional, usually a dermatologist. The process begins with a detailed review of the patient’s medical history, where they discuss symptoms, past medical conditions, and possible HPV exposure risk factors. Healthcare providers will inquire about the wart’s duration and whether you may have noticed any changes in its appearance, and they may assess if there is any pain or discomfort caused by the wart. They can also inquire about your activities such as walking barefoot in public areas since these can heighten the risk of HPV transmission. The next step in plantar wart diagnosis is a thorough physical examination.
The healthcare professional will carefully examine the soles of your feet for any evident signs of plantar warts, specifically looking for small, grainy lesions with a rough texture and the possible presence of tiny black dots. During the examination, the healthcare provider will also assess the location, size, and number of warts present. They may apply pressure to the wart as well to determine if it causes tenderness or pain, which is a characteristic feature of plantar warts. This comprehensive examination helps confirm the presence of plantar warts and aids in determining the most appropriate treatment approach for the best results.
In some cases, to confirm the diagnosis or if the appearance of the lesion is atypical, a healthcare professional may need to perform a biopsy. To do this, a small sample of the wart tissue is taken and sent to a laboratory for microscopic examination. This helps rule out other possible skin conditions such as cancer, and provides a definitive diagnosis of a plantar wart. Ultimately, a prompt and accurate plantar wart diagnosis is essential to determine both the most suitable treatment plan and prevent further spread of the virus.


There are numerous plantar wart treatment options available that are aimed at eradicating the warts and providing relief from discomfort. However, the appropriate treatment option is determined by various factors such as the wart’s size, location, and severity, as well as the patient’s medical background and preferences.
While it is advisable to seek medical advice for appropriate plantar wart treatments, a commonly used approach involves over-the-counter topical (OTC) medications containing salicylic acid. These solutions or patches gradually dissolve the wart’s layers, facilitating its removal over a few weeks, and while they are generally effective, these treatments require consistent application and may not be suitable for all cases.
Cryotherapy is another commonly chosen treatment method for stubborn or persistent plantar warts. This procedure involves applying liquid nitrogen to freeze the wart, leading to the death of the affected tissue which eventually falls off. While larger or deeper plantar warts may require repeated sessions, cryotherapy is generally effective and well-tolerated; however, some patients may experience mild discomfort during the procedure, and a blistering sensation may occur afterwards.
In cases where OTC treatments and cryotherapy have not provided satisfactory results, healthcare professionals may recommend surgical interventions instead. Curettage is a common surgical procedure for plantar warts, involving the use of a sharp spoon-shaped instrument (curette) to scrape away the wart tissue, and electrosurgery or laser therapy can be used in conjunction with this method to cauterize the blood vessels and prevent bleeding.
While surgical treatments have a higher success rate, they may require local anesthesia and the recovery time can also vary depending on the size and location of the wart.
Additionally, immune therapy – involving the application of certain substances to stimulate the body’s immune response against the wart – can be used as a treatment option. Although less commonly used than other treatments, immunotherapy can include injecting the wart with specific agents to provoke an immune reaction, which can lead to wart clearance. This plantar wart treatment method can be effective for some individuals, especially those with recurring or persistent warts, but there are other options for those with multiple or larger plantar warts that do not respond to standard treatments.
For individuals such as these, healthcare professionals may consider a combination of therapies to help eliminate the warts and provide relief. Combining different plantar wart treatments, such as topical medications, cryotherapy, and immunotherapy, can increase the likelihood of successful wart removal and reduce the risk of recurrence.
Ultimately, the best plantar wart treatment approach should be determined in consultation with a healthcare professional, ensuring that it aligns with your unique circumstances and provides the most effective and lasting solution for managing plantar warts.


Preventing plantar warts involves adopting certain measures to reduce the risk of exposure to HPV, which is the primary cause of these warts. Preventative measures are necessary to reduce the risk of developing plantar warts because the HPV strains responsible for causing these warts are highly contagious and easily transmitted.
Avoiding direct contact with surfaces in public areas where HPV may be present can be beneficial, such as swimming pools, communal showers, and locker rooms. Wearing flip-flops or other protective footwear in such places is highly recommended because it can act as a barrier between contaminated surfaces and the bare skin of the feet; therefore, protective footwear can minimize the chances of HPV transmission.
Regularly washing the feet with soap and water, particularly after spending time in public or communal areas, can help remove potential virus particles from the skin’s surface. An additional preventive measure that goes hand-in-hand with this one involves ensuring the feet remain dry and minimizing prolonged exposure to moisture, which can reduce viral growth and spread.
This includes sharing towels, socks, or shoes with individuals who have plantar warts or any other contagious foot conditions. HPV can spread through contaminated items, so using separate, clean items can greatly reduce the risk of transmission. When getting pedicures, for example, it is important to ensure that your pedicurist uses separate tools exclusively for you and does not share them with others.
It is essential to keep the skin on your feet in good condition, ensuring that it remains intact and free from cuts or abrasions. This can serve as a preventive measure by minimizing potential entry points for HPV. Proper foot care, such as moisturizing the skin regularly and protecting the feet from excessive friction or pressure, can also contribute to overall foot health and lessen the likelihood of HPV transmission.
If you already have a wart on your foot, keeping it dry can play a crucial role in preventing further spread. Moist environments can promote the growth of HPV, making the virus more contagious and increasing the risk of transmitting it to other parts of the foot or other people. By keeping the wart dry and covered, the virus’s ability to spread can be reduced, which is essential for preventing the formation of new warts.
By following these preventive measures, you can significantly reduce your risk of developing plantar warts and enjoy healthier, wart-free feet. Remember, to avoid developing plantar warts, it is essential to maintain foot health and proactively prevent possible HPV exposure. Seeking advice from a healthcare professional can offer guidance on prevention strategies and overall foot care, and getting vaccinated for HPV is also a plus!

Managing plantar warts can be a frustrating and painful experience, especially when they affect weight-bearing areas of the feet. If you have plantar warts, you should seek medical help if you notice signs of infection around the warts, such as redness, warmth, swelling, or the presence of pus, and any other concerning complications related to the warts should be promptly addressed by a healthcare professional. By seeking medical help and a medical evaluation, you can ensure a proper diagnosis and receive suitable treatment options, leading to effective management and relief from plantar warts.


Your skin health matters, so don’t delay. Our clinicians look forward to treating you and your family at one of our local New England practices.
Find Your Nearest APDerm CenterWe use cookies and other tools to enhance your experience on our website and to analyze our website traffic. For more information about these cookies and the data collected, please refer to our Privacy Policy.